No article found or not published for this site.









Recent Stories
Stories / Apr 15, 2026
BBI faculty Ricardo Araneda highlighted in Maryland Today

Stories / Jan 13, 2026
Sensor Advancement Breaks Barriers in Brain-Behavior Research

Stories / Oct 17, 2025
Art and Science of the Brain's Response to Sound

Stories / Oct 8, 2025
New Initiatives Push Toward Safe & Reliable Autonomous Systems

Stories / Sep 26, 2025
MATRIX-Affiliated Faculty Solving Challenges with Solutions...

Stories / Sep 16, 2025
Maryland Engineers Recognized with Faculty Honors

Stories / Aug 14, 2025
Ghodssi Awarded Distinguished University Professor Title

Stories / Jan 11, 2024
Xiaoming He Elected to European Academy of Sciences and Arts

Stories / Dec 21, 2023
Six Clark School Faculty Receive 2024 DURIP Awards

Stories / Dec 7, 2023
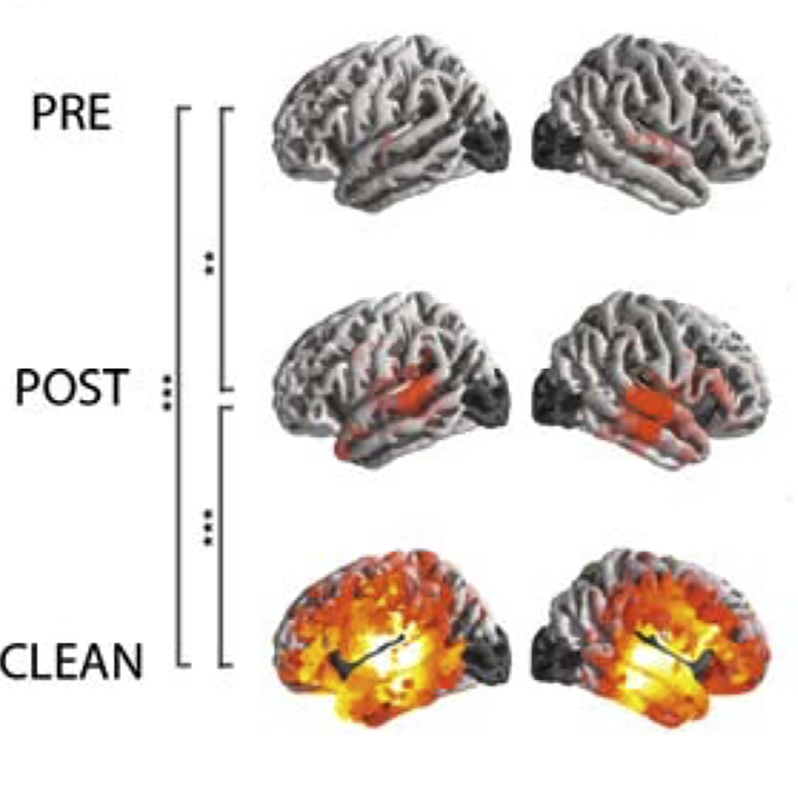
‘Priming’ helps the brain understand language even with...
